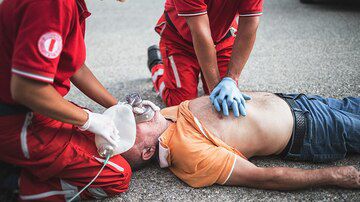
The odds of surviving out-of-hospital cardiac arrest (OHCA) are significantly better when resuscitation efforts are continued on scene, as opposed to being performed while the patient is being transported to the hospital, a large observational study has found.
The process of moving a patient during resuscitation (known as "scoop and run") may impair or delay best practices, including impairing the quality of cardiopulmonary resuscitation (CPR), say investigators with the Resuscitation Outcomes Consortium (ROC).
"Although infrequently there may be individual cases with a specific rationale to pursue hospital transport, overall, these results support a strategy that paramedics dedicate effort and expertise at the scene of the cardiac arrest, rather than prioritizing transport to hospital," first author Brian Grunau, MD, St. Paul's Hospital, Vancouver, British Columbia, Canada, told theheart.org | Medscape Cardiology.
Jeffrey M. Goodloe, MD, member of the board of directors of the American College of Emergency Physicians and chief medical officer, Medical Control Board, EMS System for Metropolitan Oklahoma City and Tulsa, agrees.
"This study supports and validates what most large urban EMS systems in the U.S. are doing, which is actively resuscitating on scene for a minimum of 20 minutes," he told theheart.org | Medscape Cardiology.
"This is absolutely in line with what we have been doing here in metropolitan Oklahoma City and Tulsa for a number of years," said Goodloe, who was not involved in the study.
The study was published online September 15 in JAMA.
The findings are based on data from the ROC Cardiac Epidemiologic Registry, which involves 10 study sites and 192 EMS agencies in the United States and Canada.
Among the full cohort of 43,969 adult EMS-treated OHCA patients (median age, 67 years; 37% women), 26% underwent intra-arrest transport. The rate of survival to hospital discharge was 3.8% among these patients, vs 12.6% among those who received on-scene resuscitation.
In a propensity-matched cohort of 27,705 OHCA patients, the probability of survival to hospital discharge was statistically significantly lower with intra-arrest transport than with continued on-scene resuscitation (4.0% vs 8.5%), an absolute difference of 4.6%, with an adjusted risk ratio (RR) of 0.48 (95% CI, 0.43 – 0.54).
Transport during resuscitation was also associated with lower probability of survival to hospital discharge with favorable neurologic outcome (modified Rankin scale, <3; 2.9% vs 7.1%), an absolute difference of 4.2%, with an adjusted RR of 0.60 (95% CI, 0.47 – 0.76).
The findings remained significant in favor of on-scene resuscitation in the subgroups of patients with initial shockable and nonshockable rhythms, as well as with EMS-witnessed and unwitnessed cardiac arrests.
SOURCE: Medscape
